TMD and Relaxation
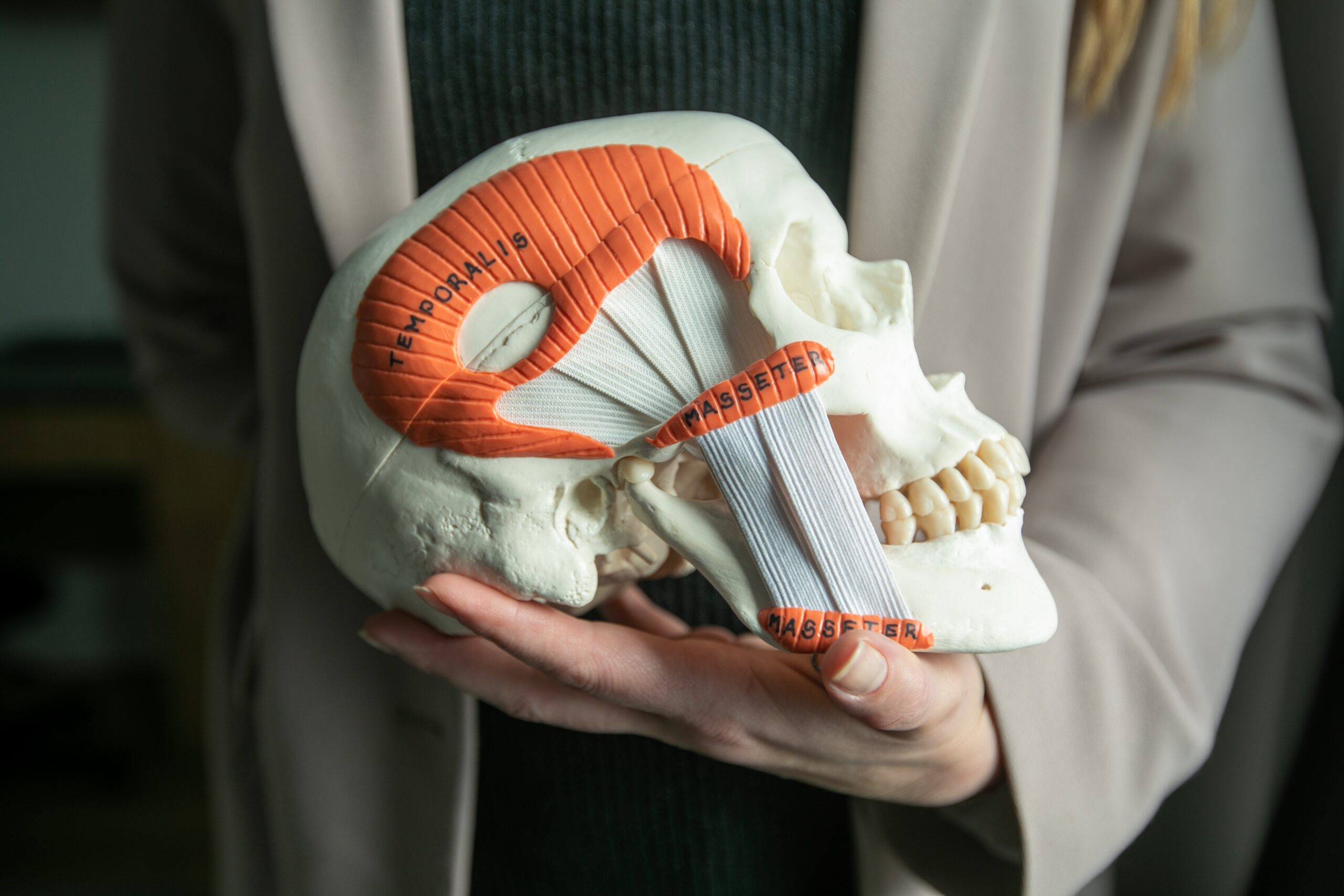
Relaxation and Meditation: A Positive Approach to Temporomandibular Dysfunction (TMD) Temporomandibular Dysfunction (TMD) refers to a set of conditions that affect the jaw joint and surrounding muscles, often leading to [...]
Should My Child Be Lifting Weights?
Is It Safe For My Child To Be Lifting Weights? As a parent, it’s completely natural to question what’s safe, what’s beneficial, and what could potentially put your child at [...]
Preventing the Return of BPPV
Can you Prevent the Return of BPPV? Benign Paroxysmal Positional Vertigo (BPPV) is one of the most common causes of dizziness. Although it’s not dangerous, it can be extremely unsettling [...]
What is the Balance Problem, BPPV?
What is BPPV? A Simple Guide to Understanding & Overcoming It Have you ever felt a sudden, spinning dizziness — often when you roll over in bed, lean down, or [...]
Rugby Injuries and How Physiotherapy Can Help
Rugby Injuries – What You Need to Know & How Physiotherapy Can Help Rugby continues to grow rapidly in the UK, with more than 880,000 players taking part across over [...]
Age-Based Plank Duration Guidelines – A Physiotherapist’s Critique
As a physiotherapist, I often work with patients who want to improve their core strength, and many of them arrive influenced by popular fitness trends in the media. One [...]
Running Injuries
Are You Ready for Marathon Season? Here's How to Stay Injury-Free As marathon season kicks off, runners of all levels are hitting the pavements and trails with renewed motivation. But [...]
Golfers Elbow
Golfers Elbow: Understanding, Diagnosing, and Treating This Common Condition As the weather begins to improve and with The Masters starting, many of us—including myself—will be eager to dust off [...]
Womens Health – The Effects of Removing Targets
How Important Are Targets? The recent decision by NHS England to remove targets aimed at reducing community waiting times and establishing women's health hubs in the 2025-26 planning guidance has [...]
Facial Muscles That Influence Temporomandibular Dysfunction (TMD)
Struggling with Jaw Pain? Our Physiotherapy Experts Can Help! Temporomandibular dysfunction (TMD) refers to a range of disorders that affect the temporomandibular joint (TMJ)—the hinge connecting your jawbone to your [...]
Understanding Bruxism and Its Impact on Temporomandibular Dysfunction (TMD)
Is Jaw Pain Disrupting Your Daily Life? We Can Help! Do you often wake up with a sore jaw or headaches? Have you noticed your teeth becoming more sensitive or [...]
Joint Health and the Gut Microbiome
Why is a Physio and not a Nutritional Therapist writing this? A few months ago, I started writing a blog post about something that kept popping up in research—how what [...]
Gut Health and Inflammatory and Autoimmune Conditions
Gut Health and Its Connection to Inflammatory and Autoimmune Conditions In recent years, research has shown that gut health plays a significant role in the development and progression of various [...]
TMD and Acupuncture
Using Acupuncture to alleviate Temporomandibular dysfunction Temporomandibular dysfunction (TMD) refers to a group of conditions that affect the temporomandibular joint (TMJ), the hinge connecting your jaw to your skull. People [...]
Shin Splints
Shin Splints: Understanding, Preventing, and Treating Medial Tibial Stress Syndrome Shin splints, medically known as medial tibial stress syndrome (MTSS), refers to both anterior and posterior shin splints. It [...]
Understanding Pelvic Organ Prolapse
Pelvic organ prolapse (POP) is a condition that affects many individuals, yet it is often underreported due to embarrassment or lack of awareness. Prolapse occurs when one or more [...]